Overview
Congestive heart failure (CHF), otherwise known simply as heart failure (HF) is the medical term that describes the heart’s inability to pump sufficiently to maintain blood flow and meet the body’s metabolic needs. This ineffective pumping leads to congestion of the venous circuit on both the pulmonary and systemic sides, leading to poor tissue perfusion and fluid overload.
Congestive heart failure results from changes in either the left or right side of the heart. This could be for example; the right side of the heart is unable to adequately clear blood from the systemic circuit, resulting in a backup of blood throughout the body. Alternatively, failure of the left side of the heart may result in fluid collecting in the lungs.
Classification
As noted above, congestive heart failure is divided into two distinct categories; left-sided heart failure, and right-sided heart failure1.
Left-Sided Heart Failure
Left-sided heart failure is an abnormal condition of the heart characterised by impaired function of the left ventricle2. If the impairment of the left ventricle is significant, the cardiac output will be greatly reduced. The increased volume and pressure on the left ventricle due its ineffective action will reflect backwards into the pulmonary circulation. the increased pressure will force fluid out of the pulmonary circulation and into the interstitium and alveoli, resulting in a crackling sound on auscultation2.
Right-sided Heart Failure
 Right-sided heart failure results from ineffective pumping of the right ventricle, resulting in venous congestion in the systemic circuit2. Right-sided heart failure will result in elevated pulmonary vascular resistance (PVR). as the PVR continues to rise, the workload of the right ventricle increases, demanding more oxygen, which may result in a thickening of the ventricle walls. As the failure continues, blood will begin to back up in the systemic circulation resulting in peripheral oedema2.
Right-sided heart failure results from ineffective pumping of the right ventricle, resulting in venous congestion in the systemic circuit2. Right-sided heart failure will result in elevated pulmonary vascular resistance (PVR). as the PVR continues to rise, the workload of the right ventricle increases, demanding more oxygen, which may result in a thickening of the ventricle walls. As the failure continues, blood will begin to back up in the systemic circulation resulting in peripheral oedema2.
Assessment
![heart failure diagram]() Left-sided Heart Failure
Left-sided Heart Failure
Nursing assessment will likely reveal the patient speaks in phrases, tachypnoeic and uses accessory muscles of respiration. There will likely be audible crackling of the lungs on auscultation, and low oxygen saturations. Tachycardia, hypotension and low capillary refill are also common.
Right-sided Heart Failure
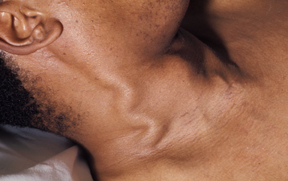
Clinically, the patient will have weight gain due to fluid retention, distended neck veins and increased jugular venous pressure (JVP), hepatomegaly and splenomegaly with dependent peripheral oedema.
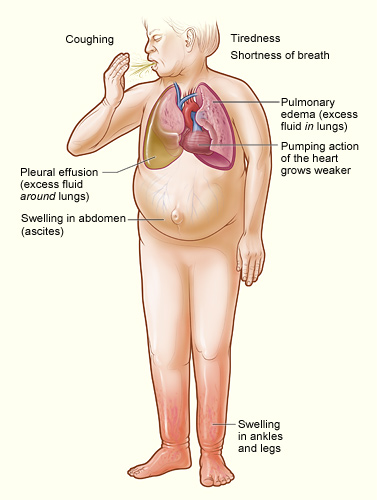
Signs and Symptoms of Heart Failure
- Dyspnea
- Lethargy
- Oedema, particularly in the legs, ankles and feet.
- Irregular tachycardia
- Decreased exercise tolerance
- Persistent cough or wheeze
- Increased nocturnal urinary urgency
- Ascites
- Lack of appetite and nausea
- Difficulty concentrating
- Chest pain (although not common in heart failure patients)
- Coughing up pink foamy mucus3
Management
Medical Management
Management of patients with heart failure will depend on the severity of their symptoms, presence of other illnesses and precipitating factors4. As congestive heart failure is not a disease in itself, there is no standard diagnosis criteria. Typically imaging studies are required, including ultrasounds to determine cardiac output. Additionally, x-rays of the chest will assist in determining if there is fluid around the lungs, and assess the condition of the cardiac walls.
Ongoing monitoring is generally carried out in the form of a fluid balance and body weight to monitor fluid shifts.
Surgical management may involve Coronary Bypass surgery, PTCA or any other innovative therapies as indicated (mechanical assist devices, transplantation)4.
Pharmacologic interventions may involve vasodilators (ACE inhibitors), ARB’s, beta-blockers, calcium channel blockers, diuretic therapy, digitalis, among others.
Patient Education
Patients may be under the belief that the heart is failing mechanically, however this is not the case. It is important to educate the patient in the physiology of the condition, explaining that the heart is failing to pump efficiently, and has not failed altogether. Congestive heart failure is not a considered a disease in itself5, but rather, the term refers to a clinical syndrome.
A person’s risk of developing heart failure in inversely related to their level of physical activity6. Patients should be encouraged to exercise and be as tolerable.
Nursing Diagnosis & Care Plan
Primary Nursing Diagnosis
Decreased Cardiac output related to an ineffective ventricular pump.
Care Plan
Nursing Diagnosis: Activity Intolerance
Goal: Participate in a desired activity, meets the needs of self-tolerance achieving increased activity can be measured, evidenced by a decrease in fatigue and weakness and vital signs during exercise7.
Nursing Interventions:
- Check vital sign before and after the activity, particularly when patients have been prescribed vasodilators or diuretics etc.
- Note the cardiopulmonary response to activity, note tachycardia, distrimia, dyspnea, sweating etc.
- Assess the precipitator and causes of weakness, for example; treatment, pain medication, shortness of breath etc.
- Evaluation of an increase in activity intolerance.
- Provide assistance in self-care activities in accordance with the indication.
Nursing Diagnosis: Excess Fluid Volume related to excess glomerular filtration rate (GFR)
Goal: Balance fluid intake and output, clean breath sounds, vital signs within an acceptable range, stable weight, no oedema. Patient educated in maintaining proper fluid balance.
Nursing Interventions:
- Monitor urine output.
- Monitor or calculate fluid balance over 24 hours.
- Maintain a sitting/semi-fowler position during the acute phase.
- Auscultation of lung sounds.
- Monitor blood pressure.
Nursing Diagnosis: Decreased cardiac Output
Goal: show vital signs are within an acceptable range, decrease dyspnoea, reduce episodes of angina.
Nursing Interventions:
- Auscultate apical pulse, assess the frequency and rythm of the heart.
- palpation of peripheral pulsees.
- Assess the skin for cyanosis and pallor.
- Provide a comfortable and quiet environment.
Image credits: OpenStax JVP | Wikimedia

 Left-sided Heart Failure
Left-sided Heart Failure
[…] The chronic inflammatory process can also lead to changes in the pulmonary vasculature, causing a thickening of the vessel lining, increasing pre-load on the right atrium of the heart, and may lead to congestive heart failure. […]