A peptic ulcer is a legion in the mucosa lining of the stomach or small intestine, allowing gastric juices to come into contact with, and damage underlying tissues. Untreated or severe peptic ulcers may lead to perforation of the stomach and spilling of gastric juices into the abdominal cavity.
Peptic Ulcers are prevalent in approximately 4% of the population1, with an estimated 10% of the population experiencing a peptic ulcer at some point in their life. In 2015 alone, over 87 million new cases were reported, resulting in a reported 267,500 deaths.
Signs and Symptoms
Patients may present with a variety of abdominal complaints, typically relating to pain and discomfort, or they be asymptomatic. In more severe cases they may present with bleeding.
- Abdominal pain strongly correlated with mealtimes.
- Bloating or abdominal fullness.
- Distension of the abdominal wall.
- Nausea or excessive vomiting.
- Loss of appetite.
- Haematemesis (blood in vomit)
- Melana (tarry foul smelling faeces)2.
Pathophysiology
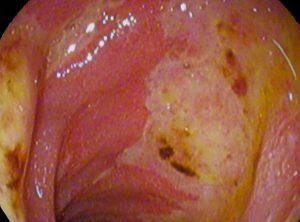
A peptic ulcer can form through a variety of physiological processes such as stress (stress ulcer), NSAIDs and colonisation by Helicobacter pylori.
The majority of ulcers have been attributed to colonisation of the antral mucosa by H. pylori, causing chronic inflammation. Due in part its location and the harsh environment of the stomach and duodenum, the body is unable to effectively respond to the infection, thus the bacterium can cause chronic active gastritis, eventually leading to the breakdown of the gastric lining.
Non-steroidal Anti-inflammatory Drugs (NSAIDs) have also been identified as another major cause of ulcers. This is due to a secondary action of many NSAIDs blocking the function of cyclooxygenase 1 (COX-1) which is essential for the production of prostaglandins which stimulate the secretion of a protective mucus. Without this mucus, the gastric mucosa is allowed to come into direct contact with the harsh gastric acids.
Dietary factors such as consumption of spices, coffee, caffeine45, and alcohol have been shown to be of relatively minor importance in the formation of peptic ulcers67.
Medical Management
Treatment typically focusses on lifestyle changes and administration of antibiotics in the case of H. pylori infections8. Cessation of smoking and alcohol consumption are typical lifestyle changes, while medications may be altered to reduce the consumption of NSAIDs. Alternatively, drugs may be prescribed to reduce the potency of gastric acids, such as proton pump inhibitors or H2 blockers1.
A bleeding ulcer may require surgery, such as an endoscopy9, while a perforation or heavily bleeding ulcer requires immediate surgical intervention to repair the site and minimise further damage by gastric juices.
Diet
Diet is not considered to play an important role in causing or preventing peptic ulcers. It is possible to minimise discomfort by avoiding foods that aggravate the ulcer.
Classification
Peptic ulcers can be categorised by either their location or by the modified Johnson scale.
By Location
| Duodenum | Duodenal Ulcer |
| Oesophagus | Oesophageal Ulcer |
| Stomach | Gastric Ulcer |
| Meckel’s Diverticulum | Meckel’s Diverticulum Ulcer |
Modified Johnson Scale
| Type I | Ulcer along the body of the stomach, not associated with acid hypersecretion. |
| Type II | Ulcer in the body of the in combination with duodenal ulcers. Associated with acid hypersecretion. |
| Type III | In the pyloric channel within 3cm of the pylorus. Associated with acid hypersecretion. |
| Type IV | Proximal Gastroesophageal Ulcer. |
| Type V | Can occur throughout the stomach typically associated with the chronic use of NSAIDs. |
Nursing Diagnosis & Care Plan
Nursing Interventions
– Record reports of pain including severity, location and duration.
– Review factors that aggravate or alleviate pain.
– Identify and limit foods that aggravate condition or cause increased discomfort.
– Encourage small frequent meals.
– Encourage patient to assume a comfortable position.
– Instruct patient to avoid NSAIDs.
Nursing Interventions:
– Assess and record body weight & Changes
– Calculate Basal metabolic needs and ensure the patient is not in a caloric deficit.
– Assist the patient in identifying foods which may irritate the ulcer, and advise them to avoid
– Educate the patient on the importance of a balanced diet.
– Assess the patient for metabolic deficits and dehydration.
Nursing Interventions
– Educate the patient or carer on the causes and processes of peptic ulcers.
– Discuss therapy options
– Instruct the patient on identifying and responding to signs and symptoms, including when and what to report.
– Explain the pathophysiology of the disease.
Nursing Interventions
– Monitor the fluid intake and output (fluid balance chart)
– Monitor the patients vital signs.
Administer IV fluids as ordered.
Nursing Interventions
– Monitor the patient for signs of Hematemesis
○ Sudden or excessively large volume of blood is a medical emergency.
– Instruct the patient to report any dark or tarry stools.
Monitor vital signs.
